
Eylea is one type of anti-VEGF injection. The other types are Avastin and Accentrix. VEGF stands for vascular endothelial growth factor. You can read more details about individual anti-VEGF drugs but Avastin usage continues to be off-label use for retinal diseases.
These anti-VEGF injections are used by eye doctors to treat eye diseases of the retina. These conditions could be age-related macular degeneration, diabetic retinal disease, or even retinal vein occlusions.
Eylea is the brand name for Aflibercept injection. It is an anti-VEGF injection, developed by Regeneron Pharmaceuticals Inc. It received FDA approval for use in the eye in 2011. Eylea is also known as VEGF Trap-Eye
VEGF or vascular endothelial growth factor is the molecule that is responsible for promoting the growth of new blood vessels and causing fluid leakage in the retina. VEGF is naturally present in the eye in diabetics and certain other conditions. Anti VEGF agents act by blocking the effects of VEGF and thus cause a reduction in the fluid and leakage and regression of new but abnormal blood vessels. As the damaged blood vessels gradually recede so does the swelling in the retina.
Aflibercept functions as a decoy receptor to sequester VEGF, thereby blocking its biological effects.
Eylea is used for the treatment of Wet ARMD (Neovascular AMD) and Macular edema due to Diabetic retinopathy and retinal vein occlusions.
ARMD stands for Age-Related Macular Degeneration. It is of 2 types :
1. In the Wet form or wet ARMD there is the formation of a neovascular membrane at the macula. This causes leakage of fluid and/or bleeding into the retina. This can cause a sudden drop in vision, or distort images. This leakage is treated by giving intravitreal Anti Vegf injection into the eye. If left untreated it can progress to scar formation and result in permanently low vision.
2. In Dry ARMD there is no leakage of fluid, however, the macula can thin out and become atrophied. There is currently no known treatment to stop the progression to atrophy, however, multivitamins can slow down the progression.
Macular edema is swelling or collection of fluid in the central part of the retina. This central part of the retina or the macula is the most important part of the retina and is responsible for most of our vision. Any disease affecting the macula significantly affects our vision. The fluid collection occurs due to 2 main reasons :
1. Vascular component – Due to release of VEGF by the diseased retina. This effect of VEGF is counteracted by anti-VEGF drugs like Accentrix, Avastin, and Eylea.
2. Inflammatory component – The diseased retina also releases different inflammatory mediators, which contribute to the swelling. This inflammatory component is treated by giving intravitreal steroids. These could be Triamcinolone or Ozurdex.
Swelling or fluid collection at the macula is commonly seen in Wet Age-Related Macular Degeneration, Diabetic Macular Edema, and Retinal Vein Occlusions like BRVO or branch retinal vein occlusions.
The current dosing schedule is 0.05 ml (2 mg) given by intravitreal injection.
a. Neovascular (Wet) Age-related Macular Degeneration (AMD): The recommended dose is 2 mg administered by intravitreal injection every 4 weeks (monthly) for the first 12 weeks (3 months), followed by 2 mg once every 8 weeks (2 months). Although Eylea may be dosed as frequently as 2 mg every 4 weeks (monthly), studies did not show additional efficacy when Eylea was dosed every 4 weeks compared to every 8 weeks. So after the first 3 doses keeping the same treatment interval did not add value and thus the treatment interval is increased to 8 weeks.
In December of 2017, Regeneron Pharmaceuticals applied for and the FDA accepted a supplemental biologics license application for 3 months dosing interval of Eylea for patients with wet age-related macular degeneration. This further reduced frequency of injection is beneficial to the Wet ARMD patients who need to take repeated injections.
b. Macular Edema following Retinal Vein Occlusion (RVO): The recommended dose is 2 mg administered by intravitreal injection every 4 weeks (monthly).
c. Diabetic Macular Edema (DME): The recommended dose is 2 mg administered by intravitreal injection every 4 weeks (monthly) for the first 5 injections, followed by 2 mg once every 8 weeks (2 months). Although Eylea may be dosed as frequently as 2 mg every 4 weeks (monthly), additional efficacy was not demonstrated when Eylea was dosed every 4 weeks compared to every 8 weeks
Eylea has 100 times more binding capacity to the receptor compared to the previous anti Vegfs agents. It also has a much longer half-life, which results in a longer duration of action. These factors result in a reduced frequency of dosing.
Eylea is an anti-VEGF drug known as Aflibercept or VEGF Trap eye. It blocks all the isoforms of VEGF, has a greater binding affinity compared to Ranibizumab, and has a longer duration of action.
1. The improved pharmacokinetics of aflibercept is thought to decrease the frequency of dosing in patients, with similar efficacy as anti-VEGF antibodies.
2. Eylea is more expensive than Ranibizumab, the MRP is double. However, because it has a longer duration of action, the frequency of injections is lesser than that with ranibizumab or Accentrix
3. It is generally reserved for those who are not responding to Accentrix, and there is a need to change the anti-VEGF.
4. However, in patients with worse vision at the beginning, Eylea shows better results than Accentrix.
a. Eylea is an intravitreal Anti-VEGF injection, which treats macular edema by blocking VEGF.
b. Ozurdex is an intravitreal steroid implant, which continues to release steroid (dexamethasone) gradually into the eye over several weeks. This steroid treats the inflammatory component in macular edema.
c. While the cost of Eylea is around Rs 65000, Ozurdex costs 35000. The effect of Eylea lasts for 6-8 weeks while ozurdex lasts for 4-6 months. However, Ozurdex has associated with the risk of causing raised eye pressure and cataracts, which is rare with Eylea. Also, ozurdex does not work in Wet ARMD.
d. In patients with diabetic macular edema and retina vein occlusions, the protocol is to start treatment with an anti-VEGF, and then switch to ozurdex if the anti-VEGF injections do not have the desired result.
As with any intraocular injection, there are some risks. The most commonly reported adverse reactions (>10%) include a slight discomfort in the eyes for a day or two, conjunctival hemorrhage, vitreous floaters, vitreous detachment, increased intraocular pressure, or glaucoma, and eye pain. Eye pain may be caused at the injection site or even due to a mild intraocular inflammation after the injection. These occasionally occur with any intravitreal injection. There can be slightly impaired vision or blurring of vision for a day or two after the injection.
Please note there are systemic side effects or fatal side effects because of these injections. Even allergies to this injection are not reported.
Severe complications are rare, and include:
Eye infection – this is known as endophthalmitis. One may experience eye pain, blurred vision, and sometimes even swollen eyelids. This is the one of most dreaded adverse effects of this or any other eye surgery or injection.
retinal detachment
cataract.
It is rare to lose vision as a result of an intravitreal injection. But if you do develop any of these Red Flag signs, then we recommend that you call our clinic immediately.
· Severe, constant pain
· New worsening pain after the first day
· Significant decrease in vision
· Severe, constant floaters
· Curtain or veil in your vision
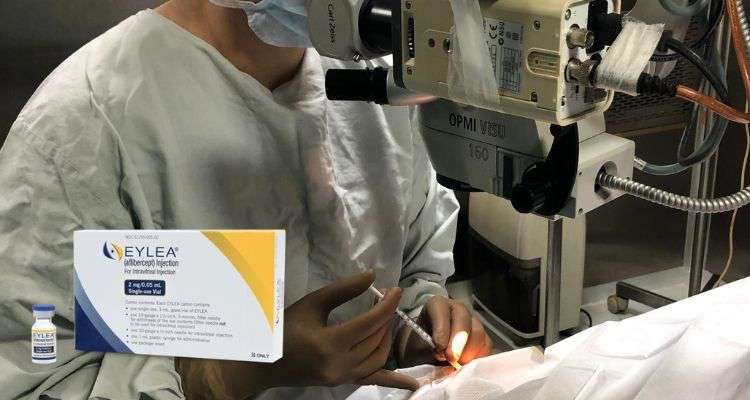
As mentioned previously this injection is given in the eye. It is given in the vitreous cavity. A patient arrives at the eye center as per the appointment. We take the patient into the operation theater. The injection procedure involves cleaning the entire half of the face on the side where the injection is planned. After covering the eye with drapes we give the eye injection under strict aseptic conditions. Eylea comes in a single-use, Glass vial and is aspirated into a tuberculin syringe. This is a thin syringe able to inject about 1ml of a drug. A 26g needle is then used to inject this drug into the eye. The amount of drug injected into the eye is 0.1ml. If your ophthalmologist feels an increase in the eye pressure after the injection he may take certain steps to reduce the eye pressure right away. Most of the time this is not necessary. The most important thing to remember here is that an aseptic injection technique should be used.
The eye is patched right after the injection. The patient can leave for home right away and the patch is removed after 2 hours. Your ophthalmologist would prescribe certain eye drops. These drops are usually antibiotics that are to be used for a week. We also ask patients to not take a head bath for 2 days after the injection.
The benefits of this injection are not visible immediately. As the macular edema reduces central vision gradually improves. The response to treatment may take 2-3 weeks and sometimes even a month. But most of the time an effect is seen in the first few weeks itself.
We usually call patients back after 2 weeks to repeat an OCT scan which will tell us exactly how much the retinal swelling has reduced. Most of the time OCT scans are repeated at monthly visits.